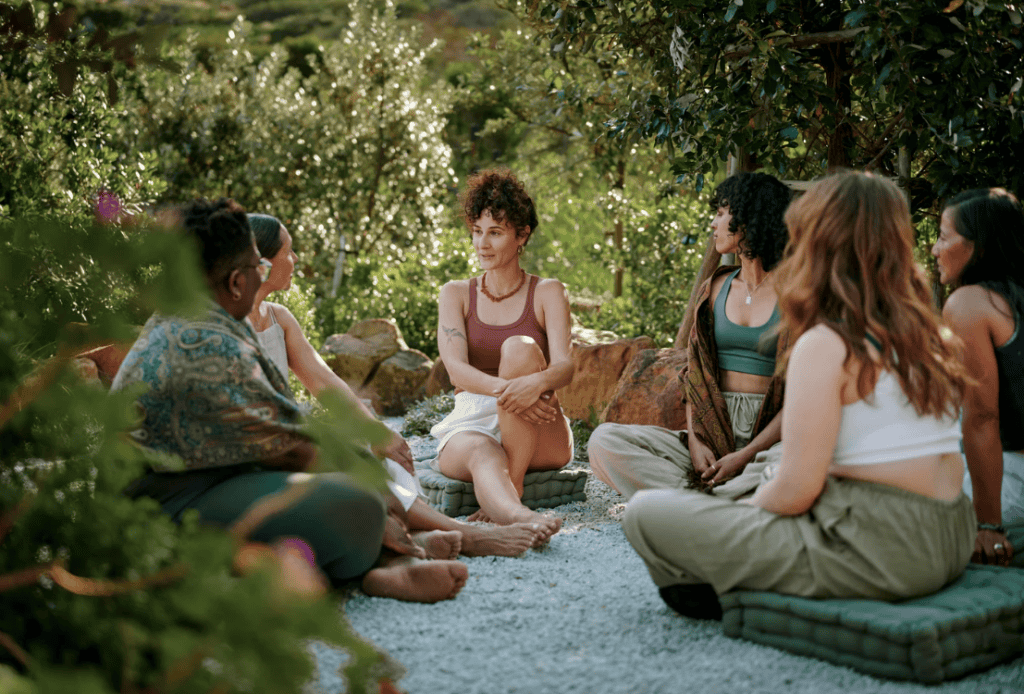Recovery isn’t a straight line.
If you struggle with addiction and have a mental illness, it can feel doubly confusing. You graduate from a residential facility… and now you’re on your own.
Here’s the problem:
That’s a big jump. And for millions of Americans, it spells disaster.
The good news? There’s a middle ground between inpatient care and independent recovery.
This article will discuss what co-occurring disorder treatment looks like in that gap, why it’s important, and how it works.
Let’s jump in!
What you’ll discover:
- What Co-Occurring Disorder Treatment Actually Means
- Why The Middle Ground Matters So Much
- How These Programs Work Day-to-Day
- Key Benefits of Stepping Down Gradually
- Choosing The Right Level of Care
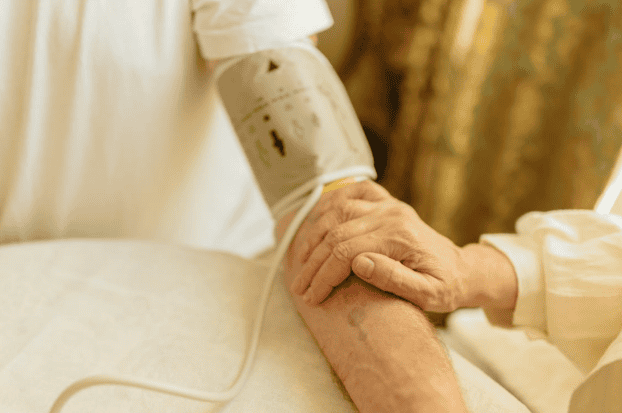
What Co-Occurring Disorder Treatment Actually Means
Integrated treatment, also known as co-occurring disorder treatment, is when you receive treatment for both a substance use disorder and mental health disorder simultaneously.
Depression and alcohol use. Anxiety and opioid dependence. PTSD and stimulant use. They fuel one another. Treating one often means the other draws the individual back.
The numbers are eye-opening.
SAMHSA reported 21.2 million adults had CODs in 20 24. That’s a lot of people who require integrated treatment… Which means not rehab only. And not therapy only. Both happening concurrently under one roof.
That’s why co-occurring disorder treatment differs from typical rehabilitation. Each program revolves around treating both disorders simultaneously.
Why The Middle Ground Matters So Much
Most people picture recovery in two extremes:
- Locked-in residential treatment
- Going home and “figuring it out”
However, much of the true, sustainable change occurs in the middle. The middle ground can be navigated with help from intensive outpatient treatment, which allows individuals to receive structured co-occurring disorder treatment without living at a recovery facility.
Why is this so important?
Transitioning from inpatient rehab is one of the most vulnerable times in sobriety. You are thrust back into your normal environment with old triggers, daily stressors, work stress, family issues. Without a routine, chances of relapse are greatly increased.
Wait…even worse. SAMHSA’s 20 24 report showed that just 14.5% of people with co-occurring disorders received treatment for both disorders. Bridging programs fill that gap.
When both conditions get attention together, recovery becomes a lot more stable.
How These Programs Work Day-to-Day
The structure is what makes the middle ground so effective.
Here’s the beauty: You come to treatment a few days a week for x amount of hours and then you go home. Sleep in your own bed and practice what you learned in the real world. That juxtaposition is what makes it so effective. You get clinical level care AND practice testing your coping skills.
A typical week in a middle-ground program for co-occurring disorder treatment might include:
- Group therapy: Where you connect with people facing similar challenges
- Individual therapy: One-on-one work with a clinician on personal goals
- Psychiatric care: Medication management for the mental health side
- Skills training: Coping tools for triggers, stress, and tough emotions
- Family sessions: Rebuilding trust and improving communication at home
The combination is important. One doesn’t work without the other. And with both addiction and the mental illness being treated together in one program … You don’t have to visit separate providers who aren’t communicating.
That kind of integrated care is hard to get any other way.
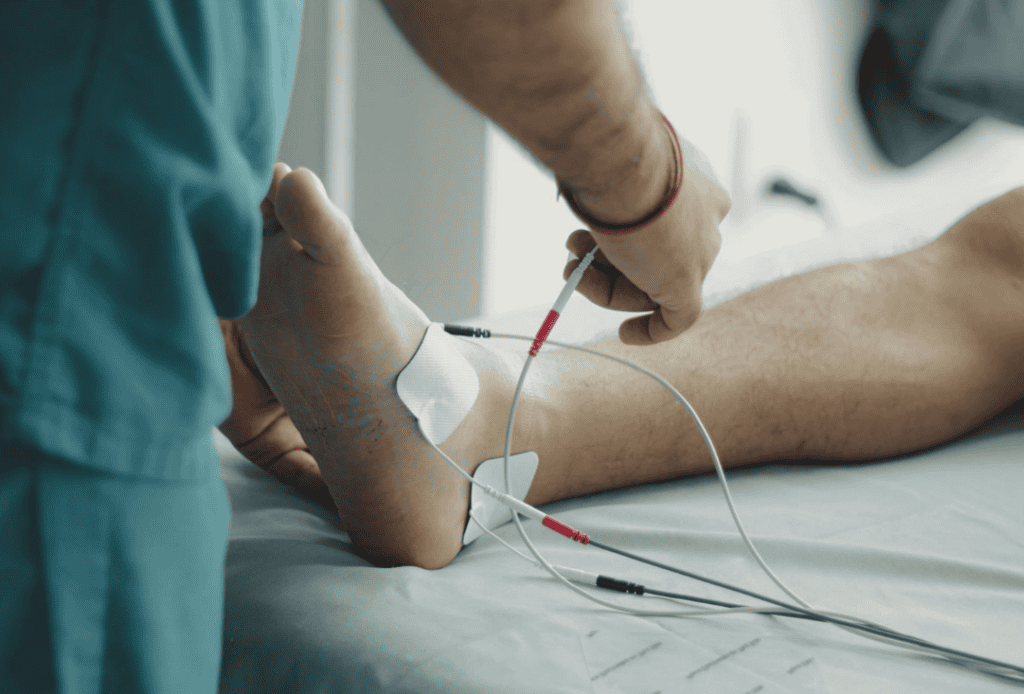
Key Benefits of Stepping Down Gradually
Clinicians recommend this type of step-down because there is a good reason. Improvements are seen in all areas of life.
Real-World Application
Inpatient care is highly controlled. Real life is not.
Mid-level programs allow you to rehearse your recovery skills with a safety net still intact. If something goes wrong on Tuesday afternoon, you can bring that issue directly into the group on Wednesday and process it with your clinician.
That kind of quick feedback loop is gold.
Lower Cost Without Lower Quality
Residential programs are expensive.
Transitioning down to outpatient level of care for COD treatment can significantly lower expenses without compromising the clinical intensity required for dual diagnosis recovery. You still have access to licensed clinicians, evidence-based treatment, and comprehensive mental health care.
You just don’t pay for the room and board on top of it.
Holding Down Daily Life
You can continue working. You can still parent. You can maintain connection to your support system.
That kind of stability is huge for long term recovery – particularly when treating addiction and a mental health issue simultaneously. Isolation from everyday life for months can be appropriate in the beginning…. But recovery has to take place in real life long term.
Better Long-Term Outcomes
Hope isn’t just a feeling — it’s a number.
74% report being in recovery from their substance use problem. Just goes to show how effective long term, comprehensive care can be. Recovering from a substance use disorder rarely happens because of one stint in treatment. It happens through a graduated system of care where dual diagnoses are treated simultaneously.
Choosing The Right Level of Care
People don’t all require the same level of intensity. The challenge is scaling care to meet where someone actually is.
Ask these questions:
- Is the person stable enough to live at home safely?
- Is there a supportive environment outside of treatment?
- Are both the addiction and the mental health condition being addressed?
- Is the program flexible enough for work, school, or family duties?
- Are the clinicians trained specifically in dual diagnosis?
So if everyone answered yes then an outpatient program is typically the safest bet following inpatient care. It’s structured enough to where change can occur, but allows for life to happen as well.
And honestly? That balance is what makes co-occurring disorder treatment actually stick.
Bringing It All Together
There shouldn’t be a void between rehab and living life on your own. There should be a transition.
Co-occurring disorder treatment in this middle ground gives people:
- Continued clinical support
- Real-world practice
- Integrated care for both conditions
- Lower cost than residential treatment
- A safer transition into independence
If you or someone you love is going through this stage, please don’t take it for granted. Active Recovery is not your Plan B – it’s usually the Plan A of recovery.
Find support, stay on the program and let God work.