Clinic planning for non-surgical facial care sits at the intersection of anatomy, patient expectations, documentation, and operational control. A strong workflow helps teams decide when to treat, when to stage care, and when to defer.
That workflow also depends on legitimate supply systems. In that wider ecosystem, MedWholesaleSupplies is a B2B supplier serving licensed clinics and healthcare professionals. It provides brand-name medical products sourced through vetted distributors and verified supply channels for licensed clinics.
Define The Clinical Scope Before Treatment Is Discussed
In practice, facial aesthetic assessment planning is not a single procedure. It is the structured assessment of facial appearance, skin quality, movement, volume, proportion, and patient goals before any intervention is selected. For clinics, the key question is not simply what can be done, but what is appropriate, safe, and likely to meet the stated concern.
It also helps to separate roles within the team. An esthetician typically focuses on skin assessment, non-invasive skin treatments, treatment preparation, and aftercare support within local rules. Facial aesthetic assessment, prescribing, injectable treatment, and management of complications usually sit with licensed clinicians whose scope permits those activities. Clear handoffs reduce confusion for patients and staff.
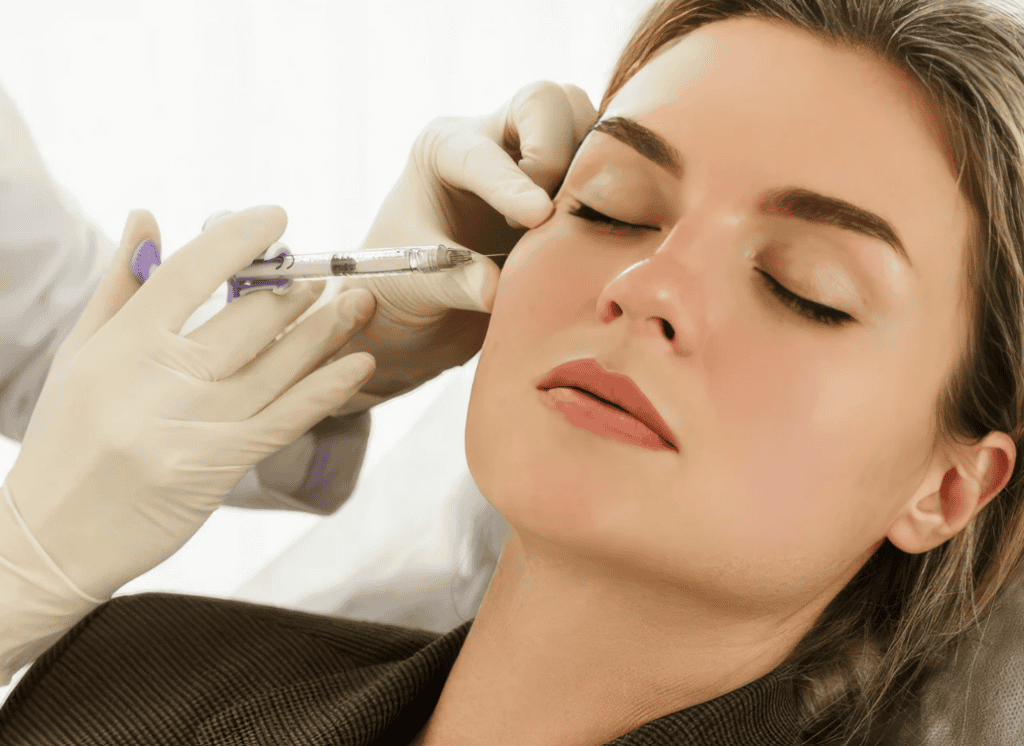
Assessment Should Uncover Fit, Risk, and Timing
The first consultation should test suitability, not just interest. Clinics usually review medical history, allergies, prior procedures, current medicines, skin disease, scar tendency, and any history that may change bleeding, healing, or infection risk. Previous aesthetic work matters because old filler, thread placement, or energy-based treatment can alter anatomy and response.
Expectation setting is equally important. Some patients describe a single feature, but the underlying issue may be broader volume loss, asymmetry, laxity, or skin texture change. Others may want same-day treatment when a staged plan or a cooling-off period would be safer. If goals are unrealistic, poorly defined, or out of proportion to the findings, deferral is a clinical decision, not a failed conversion.
Skin preparation questions should be asked early. Topical retinoids, exfoliating acids, recent waxing, peels, laser sessions, and inflamed acne can all affect barrier function and treatment timing. A routine facial may need to be modified or delayed for a patient using retinol if irritation is present, especially when the clinic is also considering resurfacing or other procedures that stress the skin.
Standardized photography and facial analysis help turn a subjective consultation into a documented baseline. Consistent lighting, resting and animated views, and notes on asymmetry or dynamic movement make later review more reliable. This also supports consent, audit, and outcome discussions.
Plan By Anatomy And Sequence, Not By Isolated Complaints
Good plans are usually built around the main driver of change rather than the most visible symptom. A complaint about lower-face heaviness may reflect midface support loss. Perioral lines may be worsened by movement patterns, skin quality, smoking history, or volume depletion. Treating a single line or fold without considering surrounding structures can create imbalance.
For that reason, many clinics use staged plans. One visit may address priority anatomy, while a later review considers whether the initial change altered the need for further treatment. This approach supports conservative endpoints and makes it easier to detect early adverse effects. It also reduces the pressure to solve a complex aesthetic concern in one session.
Documentation should record the clinical rationale, the order of treatment zones, the alternatives discussed, and the reasons for any decision to defer. In a well-run service, the plan also reflects function. Lip competence, eyelid position, lower-face movement, prior surgery, and dental or occlusal factors may all matter when appearance concerns sit close to functional anatomy.
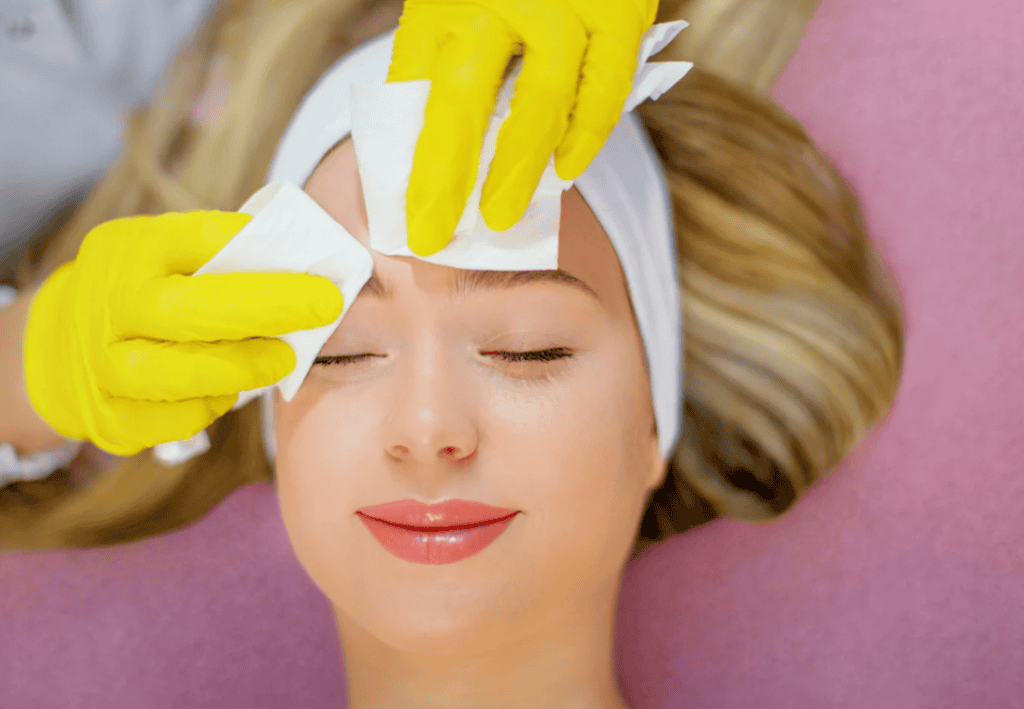
Consent And Workflow Are Part Of The Safety Case
Consent is more than a signed form. Patients need a clear explanation of intended effect, likely limits, recovery expectations, common side effects, and the clinic’s escalation plan for urgent complications. They should also understand that symmetry is rarely perfect, results may evolve over time, and additional review may be needed before any further intervention is considered.
Operational workflow should make safe practice visible. Many clinics use pre-visit screening, treatment checklists, standardized photography, batch or lot recording, sharps protocols, and written aftercare instructions. For higher-risk treatments, emergency medicines, escalation pathways, and staff drills should be defined before the clinic session begins, not improvised when a problem occurs.
If a service includes both medical treatments and spa-style skin care, scheduling rules should be explicit. Retinoid use, recent exfoliation, active dermatitis, or recent energy-based treatment may affect whether a facial, peel, or injectable session proceeds that day. This is where team communication matters: estheticians, nurses, prescribers, and front-desk staff all need the same version of the plan.
Governance, Follow-Up, and Supply Controls Support Better Outcomes
Technique matters, but governance often determines whether a clinic is consistently safe. That includes training standards, supervision, written protocols, incident review, and a low threshold for escalation when symptoms fall outside the expected course. Follow-up windows should match the treatment given and the risks involved, rather than serving as a routine courtesy alone.
Product governance is part of the same system. Clinics need clear records for sourcing, storage conditions, expiry checks, stock rotation, and lot traceability. Verified supply channels help support authenticity and recall readiness, while poor record keeping can complicate both patient care and regulatory response. These controls are especially important in services where multiple injectables, devices, and skin products may sit in the same workflow.
Access to safe care is also shaped by the wider service model. Local regulation, prescriber availability, staff competency, emergency backup, and aftercare capacity can all limit what a clinic should offer, even when patient demand exists. In that sense, planning is not only about the face in front of the clinician. It is also about whether the service around that patient is robust enough to support treatment and follow-up.
A Realistic Endpoint For Clinic Planning
The most durable facial aesthetic plans are usually modest, staged, and well documented. They prioritize anatomy, suitability, and consent over speed, and they treat deferral as a normal part of care when risk, timing, or expectations do not align. For clinics, that mindset is often the clearest marker of maturity.
Medical disclaimer: This content is for informational purposes only and is not a substitute for professional medical advice.


